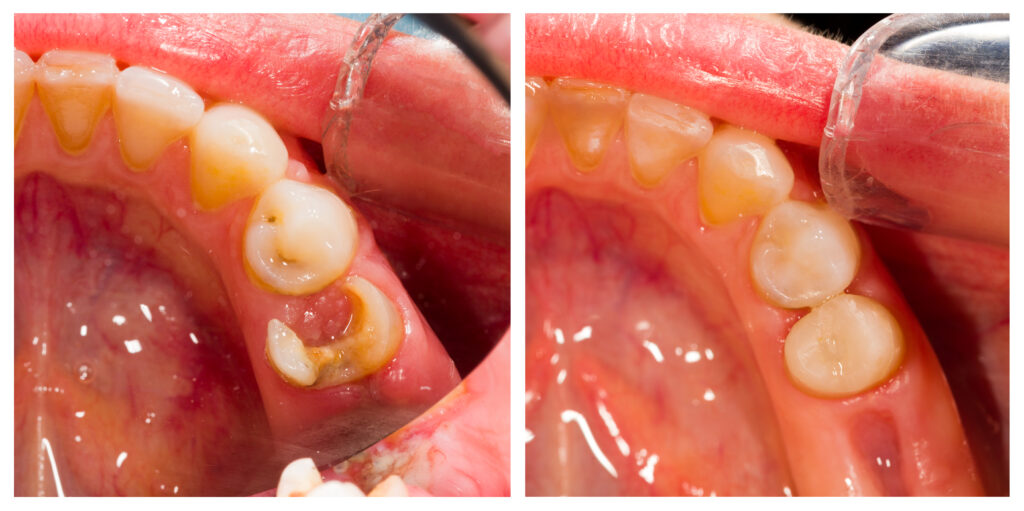
If you are preparing for a dental extraction in Singapore, it is normal to feel unsure about what will happen next. Many patients want to understand what happens during dental extraction, how to prepare for it, and what to expect after tooth extraction, especially regarding recovery and discomfort.
In this guide, we’ll outline the typical experience, including preparation, the procedure itself, and recovery. Individual experiences may vary depending on the condition of the tooth and overall oral health, so a proper dental assessment is important.
Key Takeaways
- A dental extraction procedure in Singapore is commonly performed under local anaesthesia, and patients may feel pressure but not sharp pain during removal.
- Preparing in advance with rest, soft foods, and proper planning may help make the dental extraction recovery period more manageable.
- The dental extraction recovery timeline can vary depending on whether the extraction is simple or surgical.
- Protecting the blood clot after extraction is important, as it helps reduce the risk of complications such as dry socket.
- Following your dentist’s aftercare advice may support healing and reduce the likelihood of complications.
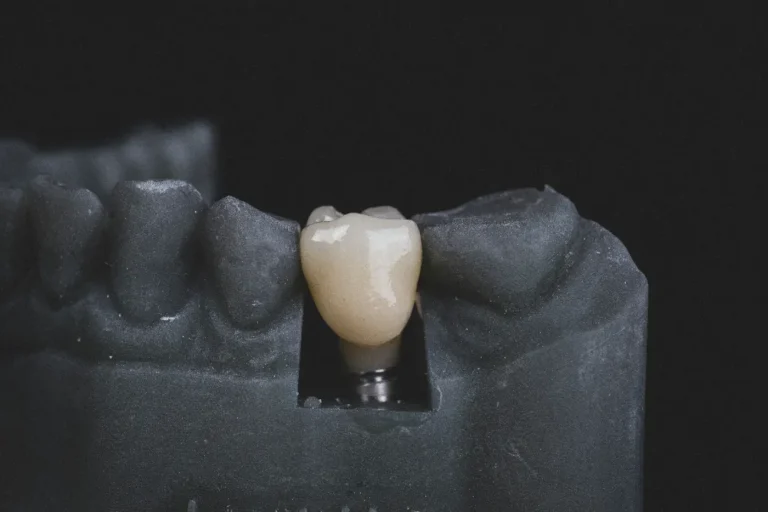
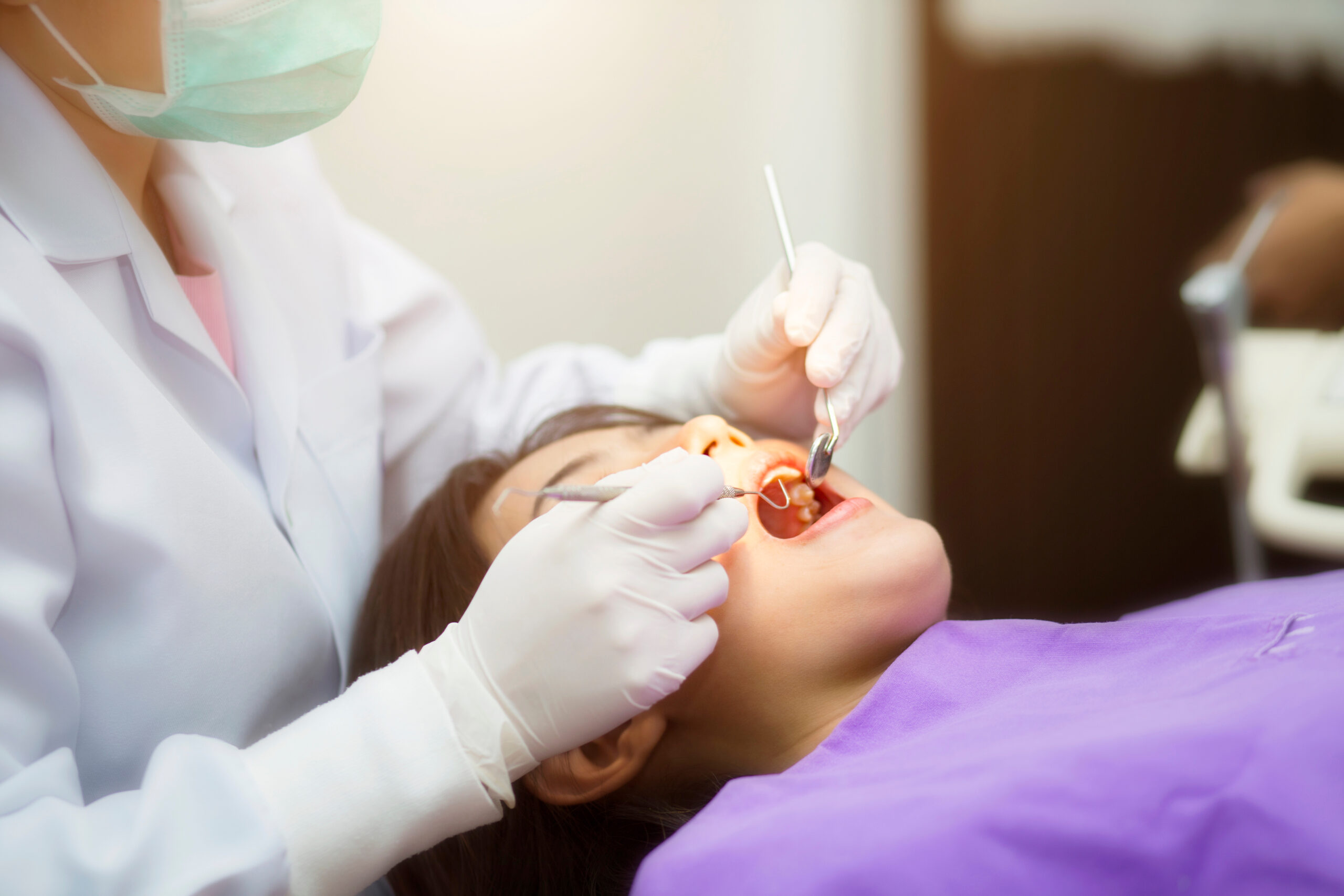
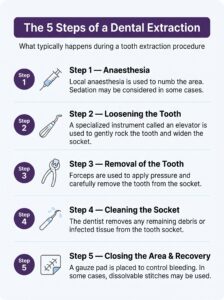
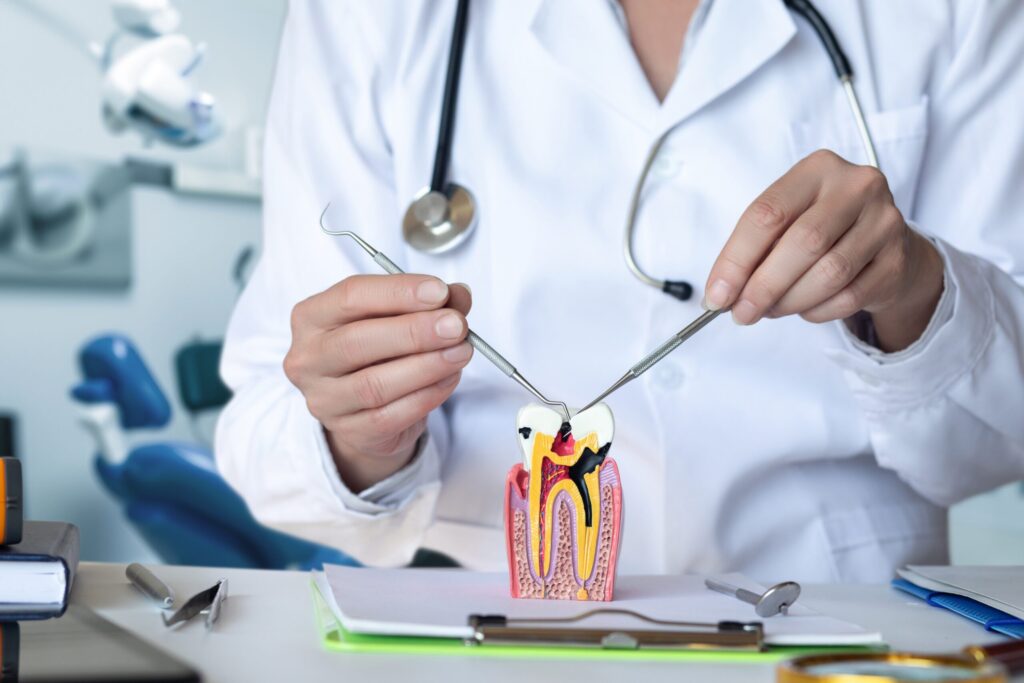
What Happens During a Dental Extraction
A tooth extraction is generally a straightforward procedure, though the exact steps depend on the tooth’s position and condition.
Many patients report feeling movement or pressure during the procedure, rather than sharp pain. The approach used will depend on your dentist’s clinical assessment.
If the extraction is simple, the steps may be quicker and involve less tissue manipulation. Surgical extractions may involve additional steps, such as a small incision or tooth sectioning. Your dentist will explain the plan that applies to your case.
Simple vs Surgical Extraction: What It Means for Your Recovery
Not all dental extractions are the same. The type of procedure can influence what you may experience during recovery.
Simple Extraction
A simple extraction is usually performed when the tooth is visible above the gum.
- No incision is required
- The procedure is generally shorter
- Recovery may be relatively quicker
Some patients can resume light activities within a few days, depending on their comfort and the dentist’s advice.
Surgical Extraction
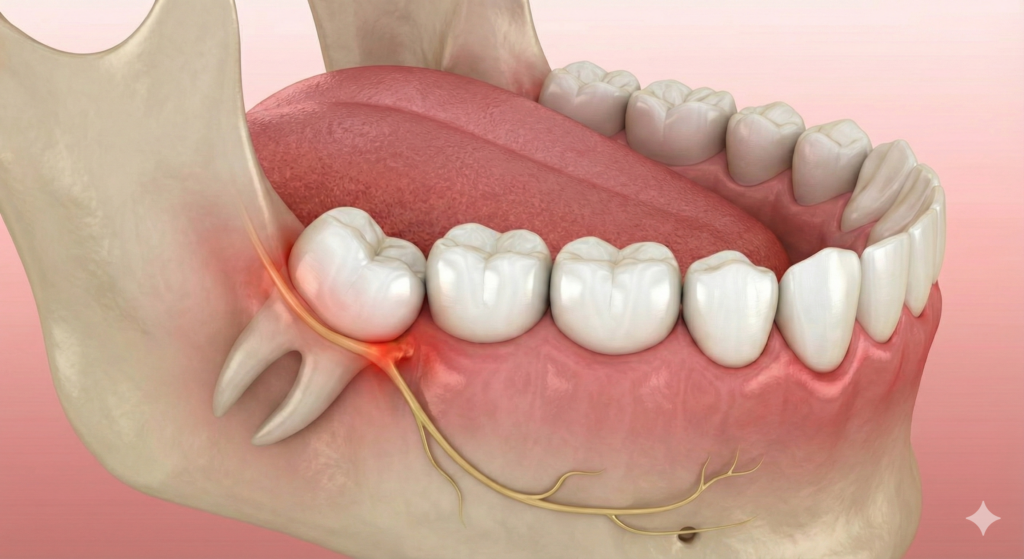
A surgical extraction may be required when the tooth is not easily accessible, such as in the case of an impacted tooth.
- A small incision may be made in the gum
- The tooth may be divided into smaller sections
- Stitches may be used
Because more tissue is involved, swelling and discomfort may be more noticeable.
Simple vs Surgical Extraction Recovery: What Feels Different
While both procedures aim to remove the tooth safely, the recovery experience may differ.
| Aspect | Simple Extraction | Surgical Extraction |
| Pain level | Usually mild | May be mild to moderate |
| Swelling | Minimal | May be more noticeable |
| Eating | May resume sooner | Soft diet may be needed longer |
| Downtime | Often shorter | May require more rest |
| Healing | Generally straightforward | May require closer monitoring |
Recovery varies between individuals, and your dentist will provide guidance based on your specific case.
How to Prepare for Dental Extraction
Preparation can influence how comfortable the recovery process feels.
Preparing for a Simple Dental Extraction
- Plan a lighter schedule for the day
- Prepare soft foods in advance
- Avoid physically demanding activities immediately after
These steps may help you rest and recover more comfortably.
Preparing for a Surgical Dental Extraction
Surgical extractions may require more preparation.
- Plan Your Recovery Time: Setting aside time to rest may help reduce strain during the initial recovery period.
- Prepare Your Diet in Advance: Soft and easy-to-eat foods such as porridge, yoghurt, and soup are commonly recommended.
- Follow Clinical Instructions Carefully: If sedation is planned, your dentist may provide fasting instructions. These should be followed closely to reduce potential risks.
Dental Extraction Recovery Timeline: What to Expect Each Day
The dental extraction recovery timeline can vary, but many patients experience the following general pattern.
First 24 Hours
- Blood clot forms at the extraction site
- Mild bleeding may occur
- Rest is recommended
Days 2 to 3
- Swelling may become more noticeable
- Discomfort may persist
- Soft foods are usually preferred
Days 4 to 7
- Swelling may begin to reduce
- Discomfort often improves
- Eating may become easier
After One Week
- Many daily activities can be resumed
- Healing continues over time
Recovery time varies depending on the complexity of the extraction and individual health factors.
Post-Extraction Care: What You Should Do for Proper Healing
After a tooth extraction in Singapore, care is focused on protecting the extraction site and supporting healing.
What to Avoid After Tooth Extraction
- Smoking or vaping
- Using a straw
- Vigorous rinsing or spitting
- Touching the extraction site
These actions may disrupt the blood clot and increase the risk of complications.
What to Eat After a Dental Extraction
Diet is an important part of recovery.
Commonly recommended foods include:
- Porridge or congee
- Yoghurt
- Scrambled eggs
- Mashed vegetables
- Lukewarm soups
Foods often avoided during early recovery include:
- Hard or crunchy foods
- Spicy or acidic foods
- Very hot drinks
- Foods with small particles
Your dentist may provide more specific dietary advice based on your condition.
Pain, Dry Socket, and What Is Normal After Extraction
Some discomfort after a dental extraction is expected, but symptoms can vary.
Normal Post-Extraction Pain
Mild to moderate soreness may occur after the anaesthesia wears off.
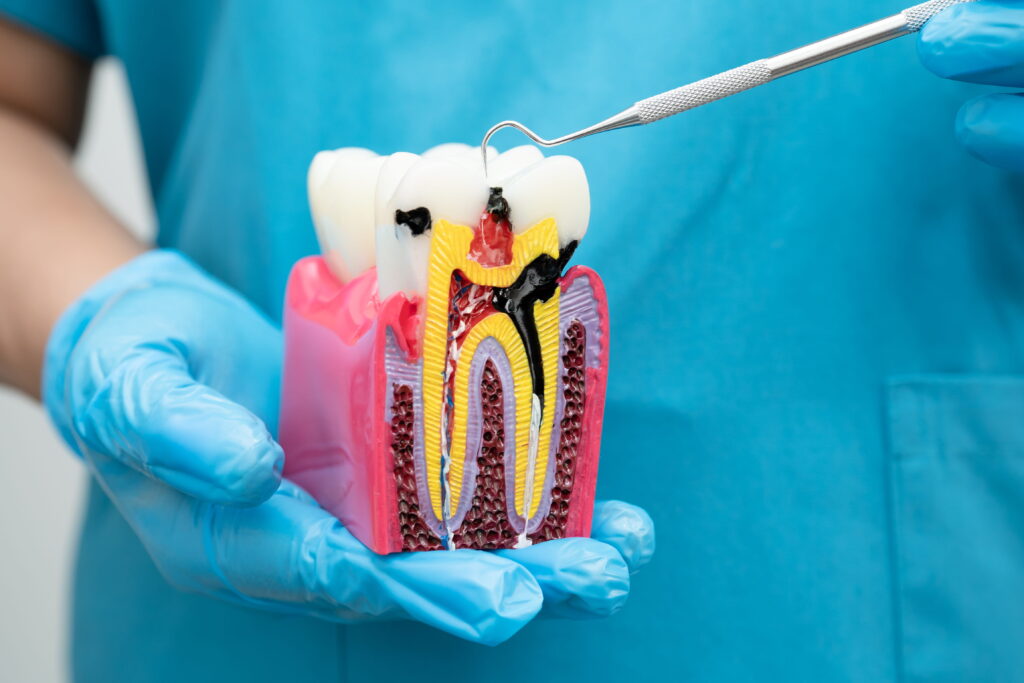
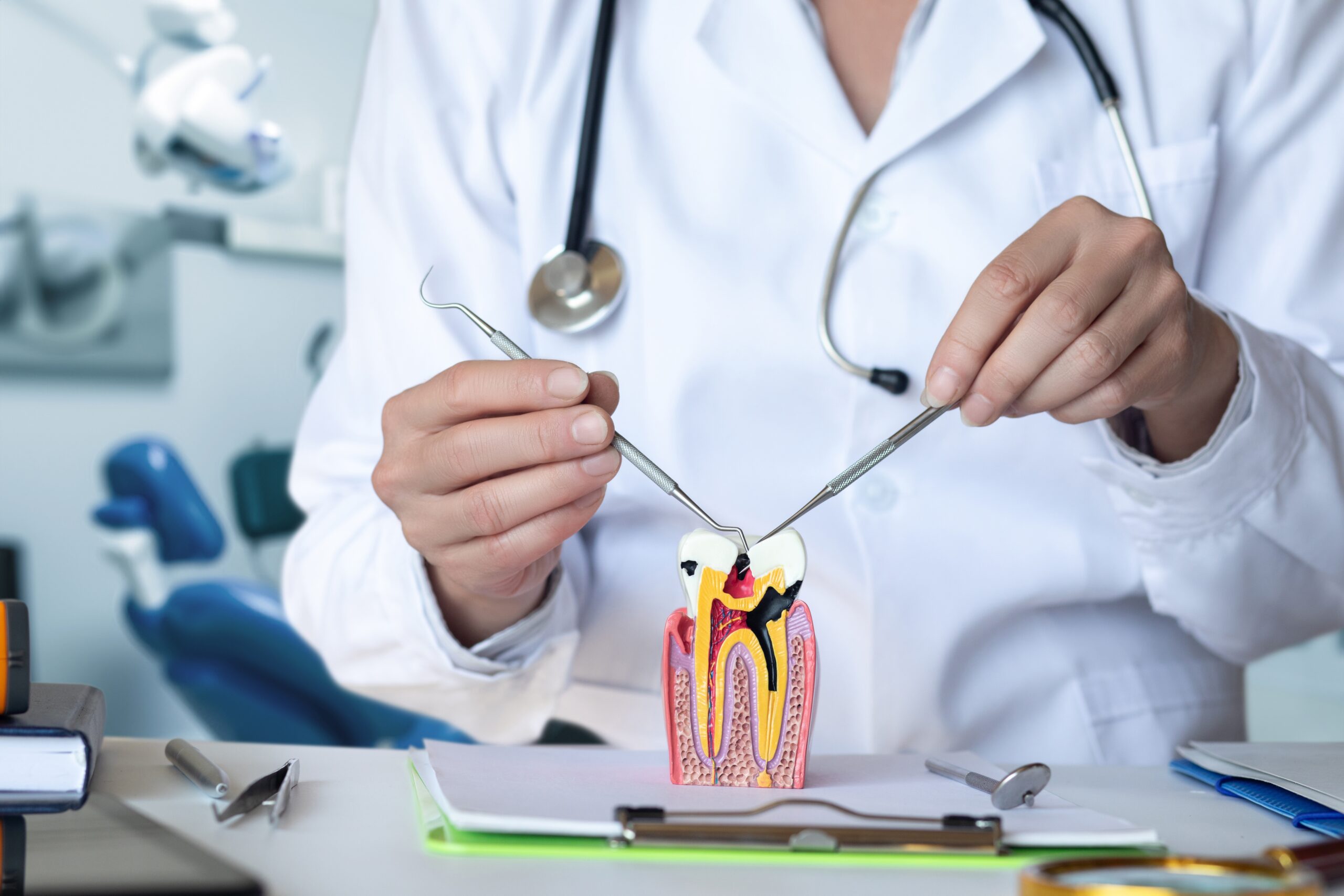
What Is Dry Socket
Dry socket can occur if the blood clot at the extraction site is lost too early.
Symptoms That May Require Attention
- Increasing or severe pain
- Unpleasant taste or odour
- Pain spreading beyond the extraction site
If you experience these symptoms, it is advisable to contact your dental clinic.
Common Recovery Mistakes That May Delay Healing
Certain behaviours may affect healing after a dental extraction.
- Returning to strenuous activity too early
- Eating hard or unsuitable foods
- Smoking during the healing period
- Not following aftercare advice
Avoiding these may help reduce the risk of complications.
When to Contact a Dental Clinic in Singapore
While many recoveries are uneventful, some symptoms should be reviewed by a dentist.
- Persistent bleeding
- Increasing swelling or pain
- Fever or signs of infection
- Difficulty opening the mouth
Early assessment may help prevent further complications.
Unsure If You Need a Dental Extraction in Singapore
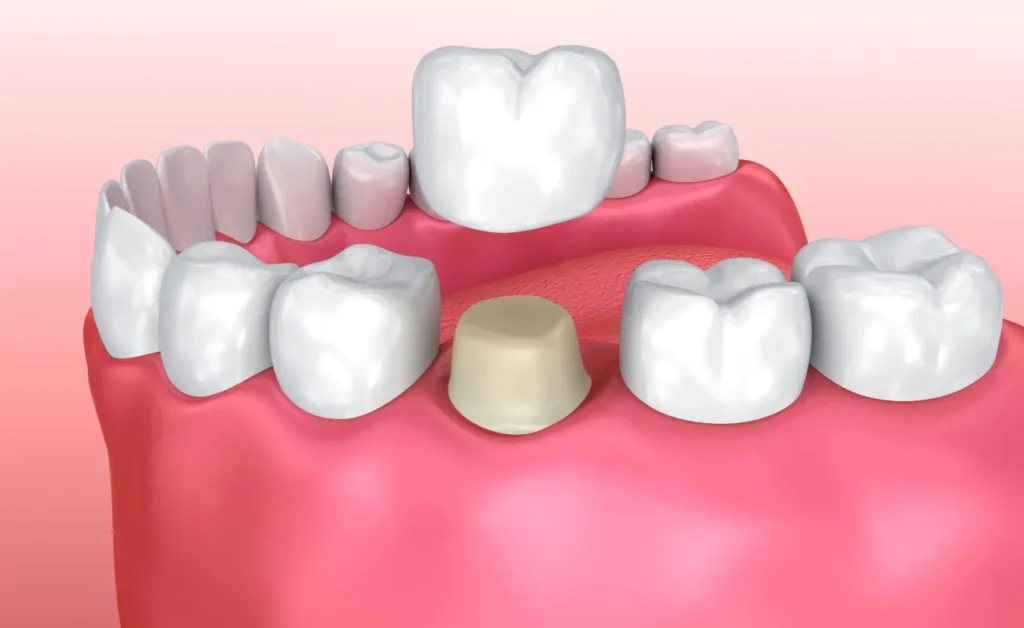
If you are unsure whether your tooth can still be saved with treatments such as a filling, crown, or root canal, it is advisable to seek a professional evaluation.
A dental assessment allows your dentist to recommend options based on your individual condition.
Dental Extraction Aftercare and Recovery Support in Singapore
Recovering from a dental extraction procedure in Singapore involves understanding what to expect and following appropriate aftercare guidance. Each patient’s experience may differ, depending on the type of extraction and overall oral health.
At Elements Dental, we support patients by explaining treatment options, outlining what to expect after tooth extraction, and providing guidance tailored to individual needs. If you are considering a dental extraction or would like to better understand your condition, you may arrange a consultation for a clinical assessment and personalised advice.
Frequently Asked Questions
Can I brush my teeth on the day of extraction
You may brush your teeth, but it is generally advised to avoid the extraction site initially and follow your dentist’s guidance.
Is it normal to feel tired after a dental extraction
Some patients may feel tired after the procedure, particularly if sedation is used or if the procedure was complex.
Can I drink cold beverages after extraction
Cold beverages are usually acceptable, but using a straw is often discouraged during early recovery.
Will stitches need to be removed after extraction
Some stitches dissolve on their own, while others may require removal depending on the material used.
How soon can I return to exercise after extraction
Light activity may be resumed depending on comfort, but strenuous exercise is often delayed based on your dentist’s advice.
Note: This article is intended for general educational purposes and is not a substitute for professional dental advice. A clinical assessment is needed before any treatment decision is made.

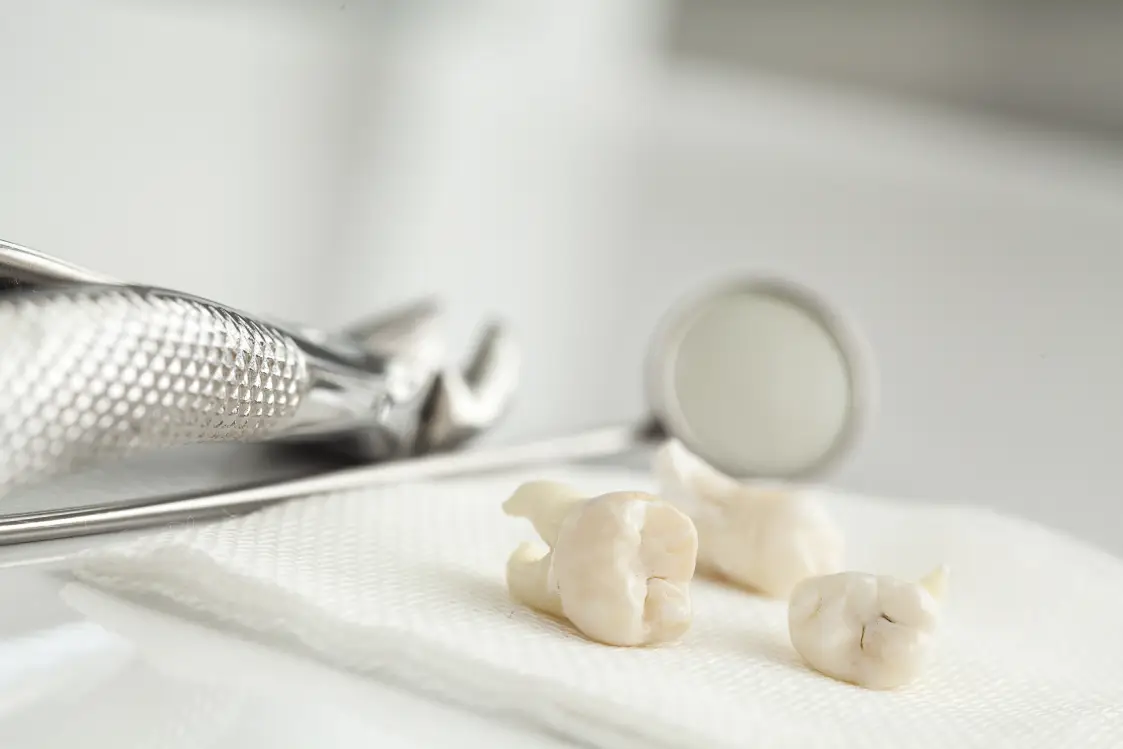

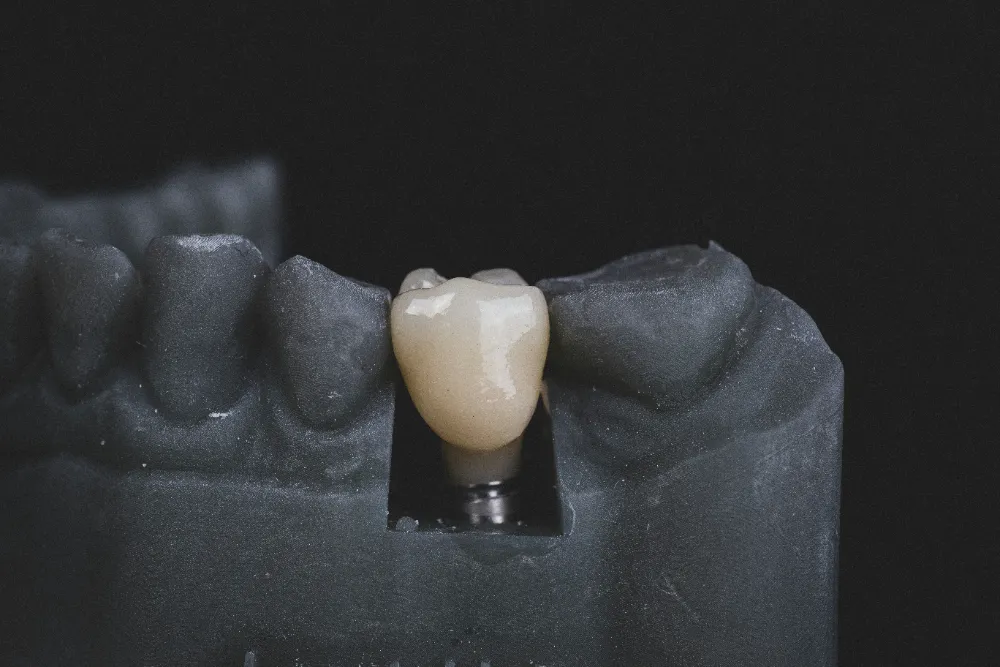
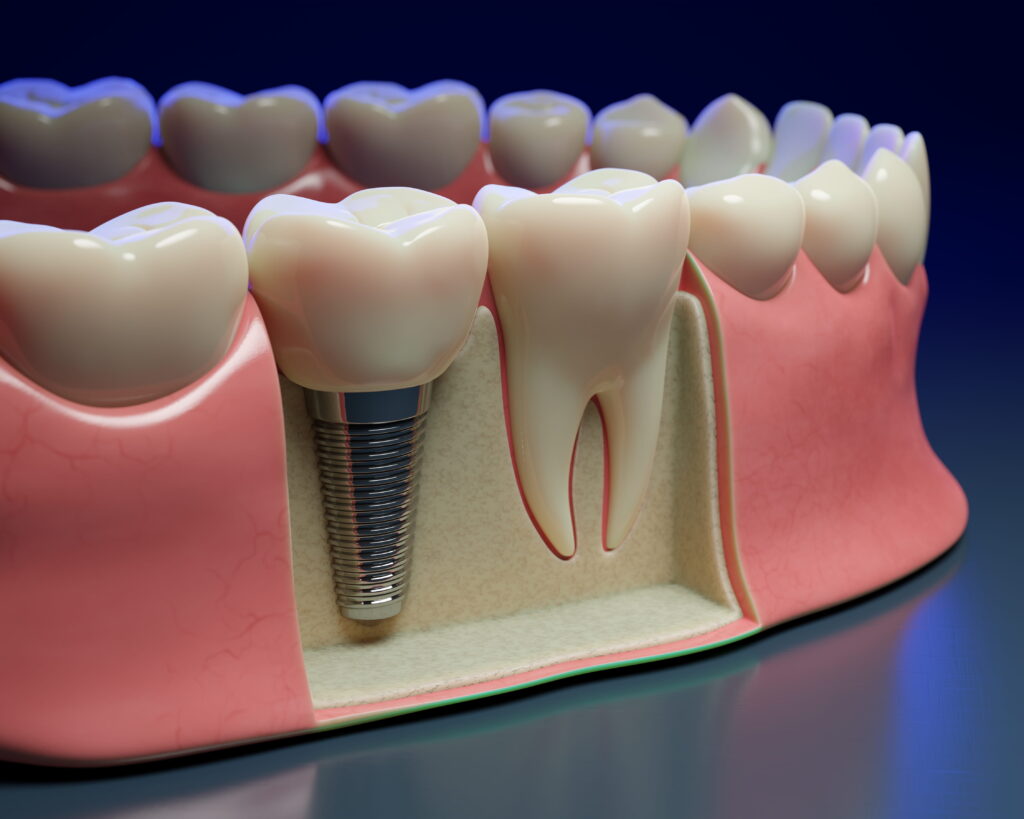
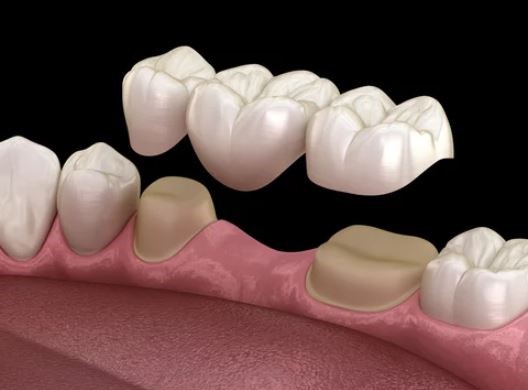
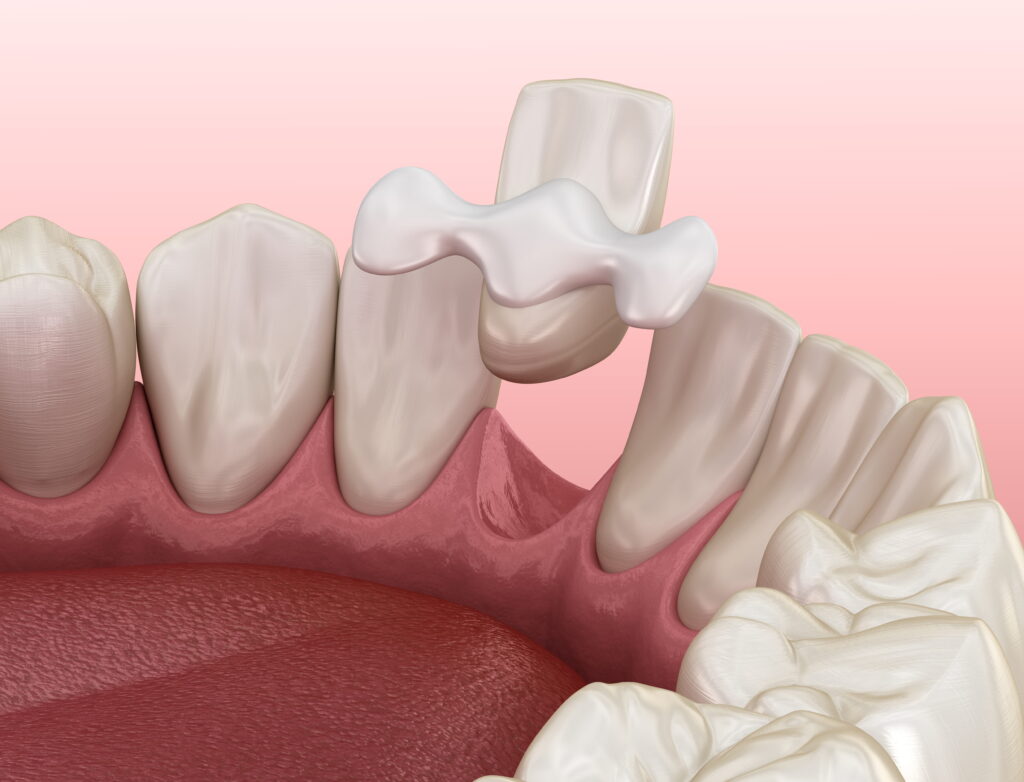


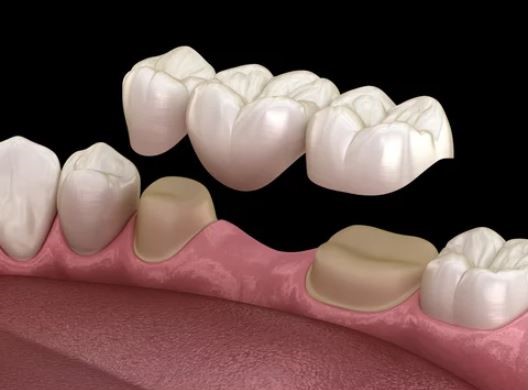

 Wisdom tooth removal refers to the extraction of the third molars—the last set of adult teeth to emerge. Because these teeth erupt after most of the jaw has finished developing, there may be limited space for them to come in properly.
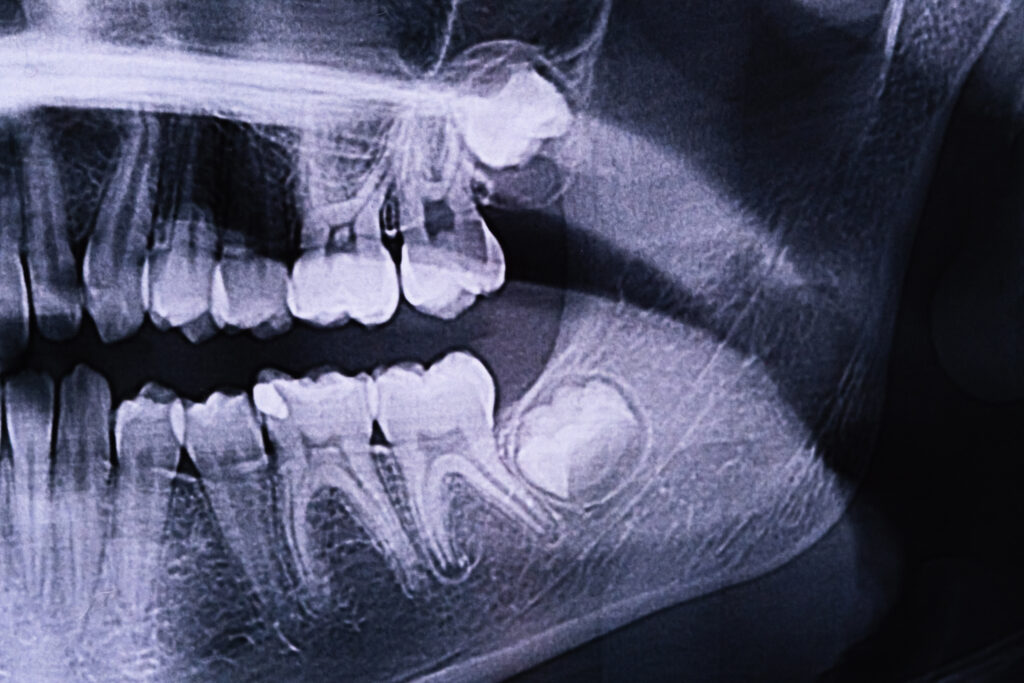
Wisdom tooth removal refers to the extraction of the third molars—the last set of adult teeth to emerge. Because these teeth erupt after most of the jaw has finished developing, there may be limited space for them to come in properly.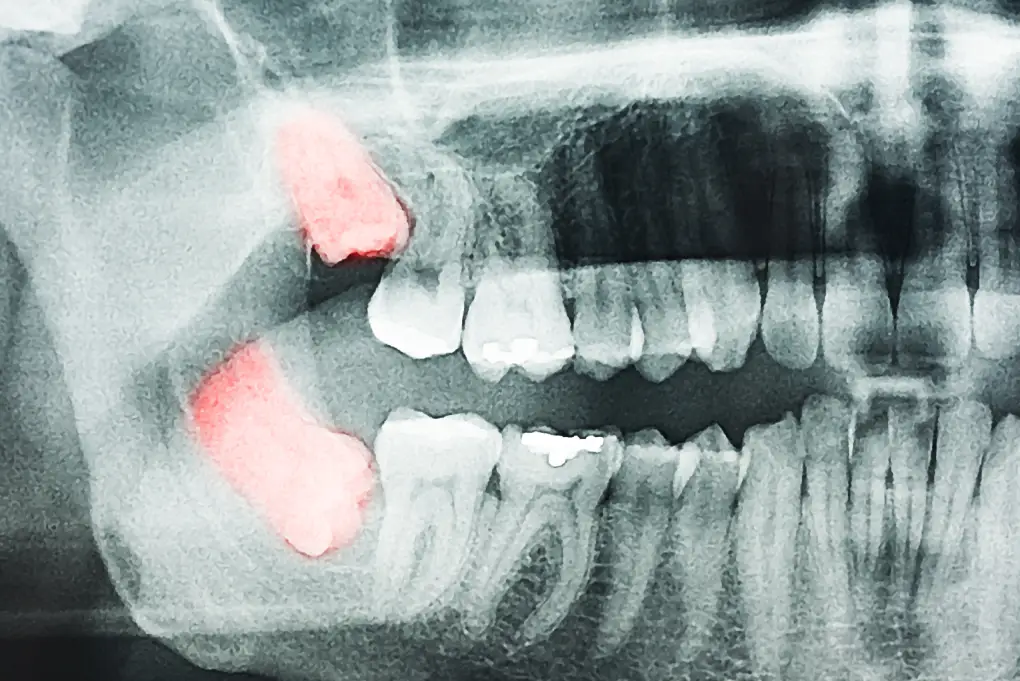 During a consultation, your dentist may recommend an X-ray to assess the position of the wisdom tooth, its relationship to adjacent teeth, and proximity to nearby nerves or sinuses.
During a consultation, your dentist may recommend an X-ray to assess the position of the wisdom tooth, its relationship to adjacent teeth, and proximity to nearby nerves or sinuses. Many cases can be managed by a general dentist. However, more complex impactions may be handled by an oral surgeon or a dentist with advanced surgical experience, which may influence professional fees.
Many cases can be managed by a general dentist. However, more complex impactions may be handled by an oral surgeon or a dentist with advanced surgical experience, which may influence professional fees. After wisdom tooth removal, most patients are advised to stick to a
After wisdom tooth removal, most patients are advised to stick to a  If you are considering wisdom tooth removal in Singapore, the process typically begins with an assessment to determine whether a simple extraction is sufficient or surgical removal is required.
If you are considering wisdom tooth removal in Singapore, the process typically begins with an assessment to determine whether a simple extraction is sufficient or surgical removal is required. Once swelling begins to settle, warm compresses may help with jaw stiffness and soreness. The timing varies by patient, so follow your dentist’s instructions.
Once swelling begins to settle, warm compresses may help with jaw stiffness and soreness. The timing varies by patient, so follow your dentist’s instructions.